Sleeve Gastrectomy is one of the most popular bariatric surgeries in the world today. While it helps countless individuals achieve substantial and sustained weight loss, it also introduces a curious and often frustrating side effect gastroesophageal reflux disease, or GERD. Many patients who once experienced no reflux at all find themselves battling frequent heartburn, regurgitation, and discomfort after surgery. But why does GERD occur after Sleeve Gastrectomy, and what can be done about it?
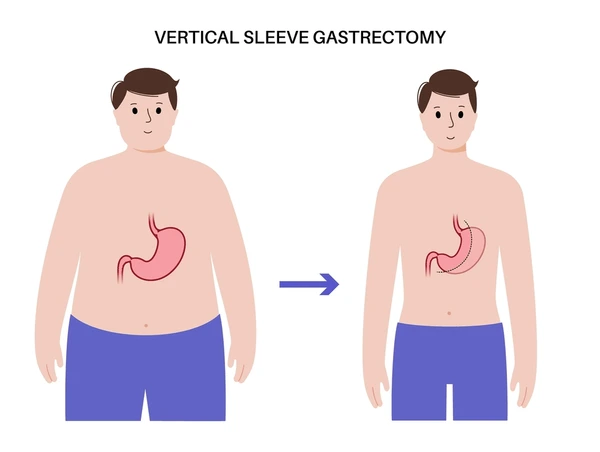
The answer lies in the intricate anatomy of the stomach and esophagus. During Sleeve Gastrectomy, nearly 80% of the stomach is removed, leaving a narrow, tube like pouch. This change not only restricts food intake but also alters the internal pressure dynamics of the digestive system. The new “sleeve” shape may cause the lower esophageal sphincter (LES) the muscular valve preventing stomach acid from rising to weaken or malfunction. As a result, acid reflux becomes a common post surgical companion.
While GERD after Sleeve Gastrectomy can be unsettling, it’s not an inevitable fate. Understanding how and why it develops is the first step toward controlling it and possibly preventing it altogether.

How Sleeve Gastrectomy Changes the Stomach
To grasp why GERD is so frequent after Sleeve Gastrectomy, it’s essential to look at what actually happens inside the body. Before surgery, the stomach is shaped like a pouch with a broad upper section that naturally accommodates meals and absorbs pressure changes. After surgery, that pouch becomes a tight vertical tube a configuration that affects how food moves and how acid behaves.
Imagine turning a balloon into a straw. The new shape creates higher internal pressure. When this pressure increases, any weakness in the LES allows acid to escape upward into the esophagus. Moreover, during Sleeve Gastrectomy, the fundus the top curved portion of the stomach responsible for producing ghrelin (the hunger hormone) and for acting as a reservoir is mostly removed. Without it, the stomach loses some of its flexibility, and the pressure from swallowed food and liquids pushes more easily against the sphincter.
Clinical studies suggest that up to 40% of patients report new or worsening reflux symptoms after surgery. This statistic doesn’t mean the surgery “causes” GERD universally, but it highlights how anatomical alterations can influence the body’s natural defense mechanisms against acid.
The Silent Culprit of Post Surgery Reflux
After Sleeve Gastrectomy, internal gastric pressure becomes the silent force behind most reflux episodes. Think of it as a pressure cooker effect. With the stomach now smaller and more rigid, every bite or sip amplifies intragastric pressure. If the LES isn’t strong enough to counterbalance this pressure, acid finds an escape route upward.
There’s another factor often overlooked the angle of His. This anatomical angle between the esophagus and the stomach acts as a natural barrier against reflux. During Sleeve Gastrectomy, this angle can be altered or flattened, weakening the anti reflux mechanism even further.
Interestingly, some patients report temporary reflux symptoms that gradually fade months after surgery. This improvement might be due to adaptation as inflammation subsides and the stomach adjusts to its new structure, the body often finds a new equilibrium. However, for others, persistent GERD remains a challenge requiring medical or surgical management.
The Role of Hiatal Hernias in GERD After Sleeve Gastrectomy
A hidden factor that intensifies reflux after Sleeve Gastrectomy is the presence of a hiatal hernia. This occurs when a small portion of the stomach pushes up through the diaphragm into the chest cavity. Even a small hernia can drastically reduce LES effectiveness, creating a direct path for acid to flow upward.
What’s important to note is that many hiatal hernias go unnoticed before surgery. They might be small, asymptomatic, and undetected unless specifically searched for during imaging or intraoperative evaluation. If left untreated, they can become the main reason behind chronic post sleeve reflux.
In recent years, many bariatric centers have emphasized repairing hiatal hernias simultaneously with Sleeve Gastrectomy. This dual approach aims to minimize the risk of postoperative reflux. While not a guaranteed solution, it’s a preventive step that acknowledges the delicate interplay between stomach anatomy and reflux physiology.
How Sleeve Gastrectomy Affects Digestion Beyond Anatomy
Beyond structural changes, Sleeve Gastrectomy triggers profound hormonal and metabolic shifts. The removal of the fundus not only reduces hunger but also alters acid production and motility. Some research suggests that this hormonal shift can indirectly affect esophageal function, either increasing or decreasing the risk of GERD depending on individual physiology.
After surgery, gastric emptying typically accelerates. Food passes more quickly from the stomach into the small intestine, which might reduce reflux in some individuals. However, when this process becomes too rapid or irregular, it can cause pressure waves that push acid upward. In addition, bile reflux though less common may also develop, further complicating the post sleeve reflux picture.
The human digestive system thrives on balance. When one part of the equation changes be it through surgery, diet, or hormones the entire system recalibrates. Understanding this interconnectedness helps explain why some patients experience reflux only temporarily, while others struggle with chronic symptoms.
Lifestyle and Behavioral Triggers After Sleeve Gastrectomy
Even with perfect surgical technique, certain post surgery habits can exacerbate GERD. After Sleeve Gastrectomy, eating patterns must evolve. Patients are encouraged to eat smaller portions, chew thoroughly, and avoid drinking fluids during meals. However, not everyone follows these rules consistently and that’s often when reflux intensifies.
Common triggers include:
- Eating too quickly or consuming large bites
- Drinking carbonated beverages or alcohol
- Lying down immediately after eating
- Consuming spicy, acidic, or fatty foods
While these may sound like universal reflux triggers, their effects are magnified after Sleeve Gastrectomy because of the smaller, high pressure stomach environment. Adjusting eating behavior and posture can make a remarkable difference in symptom frequency.
Diagnosing GERD After Sleeve Gastrectomy
Sleeve Gastrectomy patients who experience persistent heartburn or regurgitation often find themselves puzzled are these normal post surgery sensations, or signs of something more chronic? Diagnosing GERD after this operation requires a careful blend of clinical observation, patient history, and specialized testing.
Most physicians start with a symptom evaluation. Patients may report burning sensations behind the breastbone, bitter taste in the mouth, or coughing at night. However, since these symptoms can overlap with other digestive issues, more objective measures are often needed. Tests like upper endoscopy (EGD), esophageal pH monitoring, and manometry can reveal acid exposure levels, motility disorders, and potential complications such as erosive esophagitis or Barrett’s esophagus.
Interestingly, reflux after Sleeve Gastrectomy can sometimes present “silently.” In such cases, the patient may not feel typical heartburn but still suffer from chronic throat irritation or hoarseness. This is known as laryngopharyngeal reflux (LPR), and it underscores the importance of thorough, personalized evaluation rather than assuming all reflux feels the same.
First Line Approaches for Post Sleeve Gastrectomy Reflux
When reflux develops after Sleeve Gastrectomy, the first step is usually medical therapy rather than further surgery. The most commonly prescribed medications are proton pump inhibitors (PPIs), which reduce gastric acid production. These medications can offer significant symptom relief and promote healing of esophageal inflammation.
However, treating GERD after Sleeve Gastrectomy isn’t always straightforward. Because the anatomy and pressure dynamics are altered, medications that worked pre surgery might not be as effective post surgery. Adjusting dosage timing, combining with H2 blockers, or exploring newer acid reducing formulations can make a difference.
In addition to medication, certain lifestyle adjustments can greatly enhance treatment outcomes:
- Elevating the head of the bed by 6–8 inches.
- Avoiding meals at least three hours before bedtime.
- Wearing loose clothing to reduce abdominal pressure.
- Incorporating mindful eating habits slow, small bites and thorough chewing.
While these may seem like small modifications, their collective impact on reflux control can be profound, especially in the sensitive post Sleeve Gastrectomy digestive system.
Advanced Options After Sleeve Gastrectomy
Unfortunately, not all patients respond adequately to medication. When GERD persists despite optimal medical management, it’s time to consider structural solutions. Several options have been developed to address reflux while preserving the benefits of Sleeve Gastrectomy.
One of the most effective interventions is conversion to gastric bypass. In this procedure, the existing sleeve is transformed into a Roux en Y gastric bypass, which diverts acid flow and significantly reduces reflux symptoms. Studies have shown remarkable symptom resolution rates in patients undergoing this conversion.
Another approach involves magnetic sphincter augmentation (LINX device) a small ring of magnetic beads implanted around the lower esophagus. It strengthens the sphincter while still allowing food passage. Although less common in post sleeve patients, it represents a minimally invasive and promising solution for those seeking to avoid another major surgery.
In very specific cases, surgeons may also perform hiatal hernia repair or fundoplication style techniques adapted to the sleeve anatomy. These procedures aim to reinforce the natural anti reflux barrier without undoing the weight loss benefits.
Nutritional Considerations in Post Sleeve Gastrectomy GERD
Nutrition plays a surprisingly powerful role in managing reflux symptoms after Sleeve Gastrectomy. Since the stomach’s capacity and acidity levels are both altered, choosing the right foods and avoiding the wrong ones becomes an essential part of the recovery journey.
Post surgery diets are often divided into stages: liquids, purees, soft foods, and eventually solids. During this transition, patients should prioritize low acid, non irritating meals. Examples include lean proteins, oatmeal, cooked vegetables, and non citrus fruits. Conversely, acidic foods (tomatoes, citrus), fried items, and caffeine rich drinks can worsen symptoms.
Below is a simple table showing reflux friendly vs. reflux triggering foods after Sleeve Gastrectomy:
| Reflux Friendly Foods | Reflux Triggers to Avoid |
| Oatmeal, boiled eggs, chicken | Fried or spicy foods |
| Non citrus fruits (bananas, melon) | Citrus, tomato based sauces |
| Herbal teas (chamomile, ginger) | Coffee, carbonated beverages |
| Steamed vegetables | Onions, garlic, chocolate |
Keeping a food diary can also help patients identify personal triggers. Sometimes, even healthy foods like dairy or certain fruits can provoke reflux depending on the individual’s digestive sensitivity.
The Psychological Dimension of GERD After Sleeve Gastrectomy
While it’s easy to focus purely on the anatomical or medical aspects, GERD also has a psychological side particularly after Sleeve Gastrectomy, a surgery that profoundly affects one’s relationship with food. Postoperative stress, anxiety, and lifestyle transitions can amplify physical sensations and increase symptom awareness.
Research in behavioral medicine has shown that stress hormones can alter stomach acid secretion and slow digestion. This physiological shift, combined with the emotional adjustment of living with a smaller stomach, can create a feedback loop of discomfort and anxiety.
Mindful practices such as deep breathing, meditation, and gentle physical activity not only support emotional well being but can also ease reflux symptoms by reducing pressure spikes and promoting smoother digestion. The body and mind, after all, share an intimate connection especially when undergoing transformative changes like Sleeve Gastrectomy.
Long Term Monitoring and Follow Up After Sleeve Gastrectomy
Because GERD can evolve over time, long term follow up is essential after Sleeve Gastrectomy. Even patients who initially feel fine may develop symptoms months or years later as their anatomy adapts. Regular check ins with healthcare providers ensure early detection of any complications such as esophagitis or Barrett’s changes.
A typical follow up schedule may include:
- Routine clinical visits at 3, 6, and 12 months post surgery, then annually.
- Nutritional blood panels to track vitamin and mineral absorption.
- Endoscopic evaluations when reflux symptoms persist beyond medication.
This proactive approach not only helps manage reflux effectively but also preserves overall digestive health ensuring that the success of Sleeve Gastrectomy remains both sustainable and comfortable.
Preventing GERD After Sleeve Gastrectomy
Preventing reflux after Sleeve Gastrectomy begins even before surgery. Surgeons today often emphasize preoperative evaluations to identify risk factors from unnoticed hiatal hernias to pre existing mild reflux. Addressing these issues proactively can dramatically reduce post surgery discomfort.
Once the procedure is complete, prevention becomes a matter of routine awareness and care. The key lies in maintaining low intragastric pressure and supporting the body’s natural anti reflux mechanisms. Small yet consistent habits can make a substantial difference:
- Eat slowly and chew thoroughly to reduce pressure buildup.
- Divide meals into five or six smaller portions instead of three large ones.
- Stay upright for at least 30–45 minutes after eating.
- Limit caffeine, alcohol, and carbonated drinks.
- Keep hydration steady throughout the day, but avoid drinking large volumes at once.
Each of these steps helps keep reflux under control without compromising the benefits of Sleeve Gastrectomy. In many cases, mindful lifestyle choices prove as powerful as medical interventions.
The Role of Body Weight and Post Surgery Adaptation
After Sleeve Gastrectomy, most patients experience rapid weight loss and with it, a significant reduction in abdominal pressure. This weight loss itself can sometimes alleviate GERD symptoms over time. However, the early postoperative period remains delicate, as the stomach and esophagus adjust to their new configuration.
During this adaptation phase, even small variations in eating behavior or posture can trigger reflux. Some patients find that once they reach a stable weight, symptoms diminish or even disappear completely. This improvement might be linked to reduced visceral fat, which otherwise compresses the stomach and increases acid exposure.
It’s also worth noting that the healing process of the stomach lining and esophagus continues for months. Patients who remain patient and consistent with their dietary habits often find themselves rewarded with smoother digestion and less reflux over time.
Innovations in Managing Post Sleeve Gastrectomy GERD
The medical field is evolving rapidly, and so is the understanding of reflux after Sleeve Gastrectomy. New research focuses on both surgical refinement and non invasive technology to minimize GERD incidence.
For example, modified sleeve techniques such as “antireflux sleeves” preserve part of the stomach’s natural curvature and the angle of His, helping maintain reflux resistance. These innovative approaches aim to balance effective weight loss with functional digestive comfort.
Meanwhile, advances in endoscopic therapies like endoluminal suturing and radiofrequency treatment are offering minimally invasive alternatives to traditional surgeries. These methods target the lower esophageal sphincter directly, reinforcing its closure without major anatomical disruption.
Researchers are also exploring personalized medicine using genetic, hormonal, and microbiome data to predict which patients are most likely to develop GERD after surgery. The future of bariatric care seems to be heading toward prevention through prediction rather than treatment after the fact.
Living Comfortably After Sleeve Gastrectomy
Behind every data point lies a personal story. For many patients, the journey after Sleeve Gastrectomy is filled with both triumphs and adjustments. Some describe their early reflux symptoms as a temporary hurdle a reminder that the body needs time to adapt to its new rhythm. Others find that once they fine tune their diet and lifestyle, life after surgery becomes more enjoyable and sustainable.
What unites these experiences is resilience. Whether through medical support, patient communities, or self awareness, most individuals learn to read their body’s signals better than ever before. Reflux, when managed thoughtfully, rarely overshadows the profound life changes that Sleeve Gastrectomy can bring.
Stories of patients who conquered chronic heartburn with simple habit shifts avoiding late night meals, staying active, and prioritizing mindfulness serve as inspiring examples. These experiences remind us that while the science behind reflux is complex, the human ability to adapt remains extraordinary.
The Interplay of Science and Lifestyle in GERD After Sleeve Gastrectomy
The relationship between Sleeve Gastrectomy and GERD illustrates a fascinating intersection of anatomy, physiology, and behavior. The surgery reshapes not only the stomach but also the entire digestive environment influencing hormones, pressure gradients, and even the microbiome. Understanding these changes requires both scientific insight and empathy toward the patient experience.
In the end, controlling reflux is rarely about one single solution. It’s about combining medical knowledge with consistent lifestyle discipline: balanced nutrition, proper hydration, mindful eating, and long term follow up. When these elements come together, the result is more than just reflux relief it’s a restored sense of comfort and confidence in one’s own body.
A Balanced Future After Sleeve Gastrectomy
As bariatric science progresses, the conversation around GERD after Sleeve Gastrectomy continues to evolve. Once considered a simple side effect, reflux is now seen as a dynamic condition that reflects how delicately the human body balances its systems after transformation.
For patients and clinicians alike, the goal is not just weight loss but quality of life a digestive system that functions comfortably, efficiently, and sustainably. With thoughtful surgical planning, personalized follow up, and educated self care, living reflux free after Sleeve Gastrectomy is not only possible but increasingly achievable.Ultimately, the story of GERD after Sleeve Gastrectomy is one of adaptation the body adjusting to change, medicine refining its techniques, and individuals discovering new ways to live in harmony with their health journey.