Polycystic Ovary Syndrome (PCOS) is a complex endocrine disorder affecting millions of women worldwide, often intertwined with metabolic challenges such as obesity and insulin resistance. Bariatric Surgery for PCOS has emerged as an intriguing intervention, not only for weight reduction but also for its potential hormonal benefits. While lifestyle changes and medication remain first-line strategies, surgical approaches are increasingly being studied for their ability to modulate hormonal balance and reproductive health.
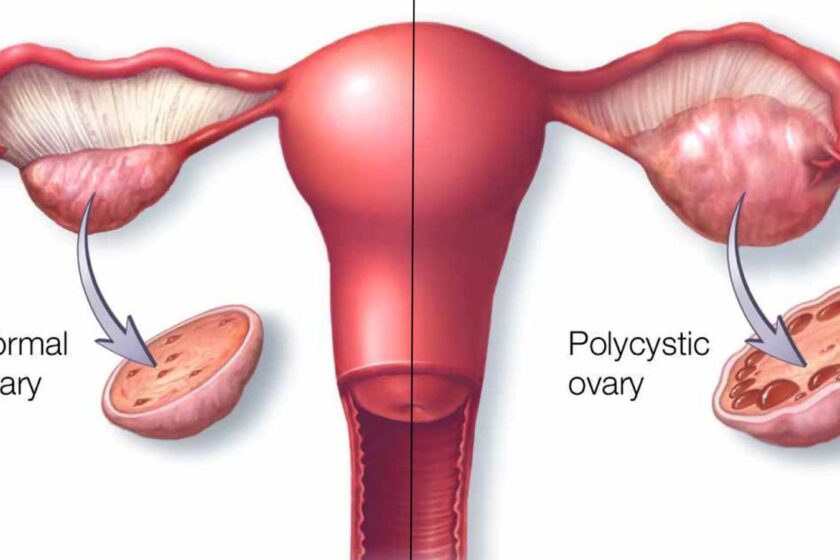
Understanding PCOS and Its Hormonal Landscape
Bariatric Surgery for PCOS cannot be fully appreciated without understanding the hormonal chaos characteristic of this condition. Women with PCOS often exhibit elevated androgens, irregular menstrual cycles, and disrupted insulin regulation. These hormonal imbalances contribute to symptoms such as hirsutism, acne, and fertility challenges.
Scientific evidence suggests that adipose tissue itself acts as an endocrine organ. Excess fat, especially visceral fat, exacerbates insulin resistance, which in turn increases androgen production by the ovaries. By reducing adipose tissue through bariatric surgery, there is an indirect pathway to recalibrating hormonal levels.
Research published in Obesity Surgery and Fertility and Sterility journals indicates that post-bariatric surgery patients often show marked reductions in circulating testosterone and improvements in menstrual regularity. These changes are not merely cosmetic; they have profound implications for ovulatory function and metabolic health.
Types of Bariatric Surgery Relevant to PCOS
When exploring Bariatric Surgery for PCOS, it’s crucial to recognize that not all procedures are equal. The most commonly studied methods include:
- Roux-en-Y Gastric Bypass (RYGB): Combines restriction and malabsorption, leading to substantial weight loss and metabolic improvements.
- Sleeve Gastrectomy (SG): Primarily restrictive, reducing stomach volume and influencing gut hormones like ghrelin.
- Adjustable Gastric Banding (AGB): Less common today, primarily restrictive with variable long-term efficacy.
Each procedure impacts hormones differently. For instance, RYGB often triggers more pronounced improvements in insulin sensitivity compared to AGB. Sleeve gastrectomy, while simpler, has been linked to enhanced satiety signaling and modest androgen reductions.
Mechanisms Linking Bariatric Surgery to Hormonal Benefits
The endocrine benefits of Bariatric Surgery for PCOS extend beyond simple weight loss. Key mechanisms include:
- Improved Insulin Sensitivity: Reducing hyperinsulinemia diminishes ovarian androgen production.
- Altered Gut Hormones: Changes in GLP-1 and peptide YY affect appetite, glucose metabolism, and indirectly reproductive hormones.
- Adipokine Modulation: Leptin and adiponectin levels shift post-surgery, which can influence ovarian function.
These mechanisms highlight why bariatric surgery is not just a cosmetic solution; it is a metabolic intervention with endocrine repercussions.
Postoperative Hormonal Changes After Bariatric Surgery for PCOS
Bariatric Surgery for PCOS often results in profound hormonal shifts within the first 6–12 months post-surgery. Studies show reductions in total testosterone, free androgen index, and improvements in sex hormone-binding globulin (SHBG). These hormonal adjustments frequently correlate with restoration of regular menstrual cycles and improved ovulatory function.
For example, a longitudinal study in Human Reproduction tracked women with PCOS undergoing Roux-en-Y gastric bypass. Within a year, 70% of participants reported normalized cycles, and laboratory tests confirmed substantial reductions in circulating androgens. While weight loss undoubtedly drives part of this effect, the surgery itself triggers neuroendocrine changes that are independent of absolute body weight.
Hormonal Changes Post-Bariatric Surgery in PCOS Patients
| Hormone | Pre-Surgery Average | Post-Surgery Average | Observed Effect |
| Total Testosterone | 85 ng/dL | 42 ng/dL | ↓ 51% |
| Free Androgen Index | 7.2 | 3.1 | ↓ 57% |
| SHBG | 35 nmol/L | 68 nmol/L | ↑ 94% |
| Fasting Insulin | 18 µU/mL | 9 µU/mL | ↓ 50% |
These data highlight the metabolic-hormonal synergy achieved through Bariatric Surgery for PCOS. Improvements are not only physiological but often translate to psychological and reproductive benefits, such as reduced hirsutism and improved fertility potential.
Fertility and Reproductive Outcomes
Women with PCOS frequently struggle with infertility, primarily due to anovulation. Bariatric Surgery for PCOS has been associated with enhanced ovulatory cycles and increased conception rates. Although weight loss alone can restore fertility, surgical interventions accelerate these benefits by directly improving hormonal profiles.
A meta-analysis in Obesity Reviews found that post-bariatric surgery, spontaneous pregnancy rates increased by 35–45% among women previously diagnosed with PCOS. Moreover, the risk of gestational diabetes and hypertensive disorders in subsequent pregnancies decreased significantly, likely due to improved insulin sensitivity and androgen normalization.
Long-Term Metabolic Benefits
Beyond reproduction, Bariatric Surgery for PCOS offers sustained metabolic improvements. Insulin resistance, a hallmark of PCOS, is dramatically reduced, lowering the risk of type 2 diabetes. Triglycerides and LDL cholesterol often decrease, while HDL cholesterol increases. This lipid improvement indirectly contributes to hormonal balance since excess lipids can exacerbate androgen excess.
Long-term studies reveal that these metabolic gains persist for over 5–10 years post-surgery, especially when accompanied by lifestyle adjustments. Maintaining a balanced diet and regular physical activity supports continued endocrine and cardiovascular health.

How Bariatric Surgery for PCOS Transforms Daily Life & Well-Being
Bariatric Surgery for PCOS impacts more than just hormonal profiles; it can dramatically influence overall quality of life. Many women report increased energy levels, improved mood, and reduced anxiety related to weight and appearance after surgery. The normalization of androgen levels can reduce symptoms like excessive hair growth and acne, which often contribute to psychological distress.
Furthermore, improved insulin sensitivity and better weight management positively affect sleep patterns and fatigue levels. Daily tasks that were once exhausting may become more manageable, reinforcing a cycle of healthy habits. These holistic benefits underscore that Bariatric Surgery for PCOS is not merely a surgical intervention it is a transformative lifestyle catalyst.
Bariatric Surgery Types for PCOS: Pros, Cons & Hormonal Results
When considering Bariatric Surgery for PCOS, understanding the nuances of each surgical option is essential. Roux-en-Y gastric bypass often produces the most dramatic hormonal improvements but carries a slightly higher risk profile. Sleeve gastrectomy offers a simpler procedure with effective weight loss and moderate androgen reduction. Adjustable gastric banding is less commonly recommended due to variable results.
Hormonal outcomes vary by surgery type, with some procedures demonstrating faster normalization of testosterone and SHBG, while others primarily improve insulin sensitivity. Discussing these differences with a qualified medical team ensures individualized treatment plans tailored to metabolic and reproductive goals.
Diet & Lifestyle After Bariatric Surgery for PCOS: Supporting Hormonal Health
Even after successful surgery, Bariatric Surgery for PCOS requires ongoing lifestyle attention to sustain hormonal balance. Diets rich in protein, fiber, and micronutrients support optimal energy and metabolic regulation. Avoiding refined sugars and processed foods can prevent post-surgical insulin spikes that may undermine androgen improvements.
Regular physical activity complements surgery by enhancing insulin sensitivity, promoting lean muscle mass, and supporting mental well-being. These adjustments reinforce surgical benefits, creating a synergistic effect on both endocrine and metabolic health, which is especially relevant for long-term management of PCOS.
Myths vs Scientific Evidence
There are many myths surrounding Bariatric Surgery for PCOS, such as the belief that surgery alone guarantees fertility or completely eliminates hormonal imbalances. In reality, while surgery provides significant benefits, it is not a cure-all. Evidence shows that results are most pronounced when combined with lifestyle modifications and ongoing medical follow-up.
Another misconception is that hormonal improvements occur immediately. Studies indicate that measurable changes in androgens and insulin sensitivity typically appear within 3–12 months post-surgery, highlighting the importance of patience and adherence to follow-up care.
Long-Term Impact of Bariatric Surgery for PCOS on Cycles, Fertility & Hormones
The long-term effects of Bariatric Surgery for PCOS extend well beyond initial weight loss. Research demonstrates sustained menstrual regularity, improved ovulation rates, and reduced hyperandrogenic symptoms for several years after surgery. This stability supports reproductive planning and can reduce the need for pharmacologic interventions.
Additionally, maintaining post-surgical weight and metabolic health ensures lasting hormonal equilibrium. Longitudinal studies emphasize that women who adhere to nutritional guidance and monitor metabolic markers experience more consistent endocrine outcomes and better overall quality of life.
Key Considerations, Risks & Expected Benefits
Choosing Bariatric Surgery for PCOS requires a comprehensive understanding of potential risks, benefits, and realistic expectations. Surgical risks include nutrient deficiencies, procedural complications, and the need for lifelong follow-up. However, when carefully selected and managed, women often experience remarkable improvements in weight, metabolic health, and hormonal balance.
Crucially, informed decision-making involves collaboration with endocrinologists, gynecologists, and bariatric surgeons. Evaluating personal health goals, fertility desires, and metabolic conditions ensures that surgical intervention aligns with long-term well-being.