Bariatric Surgery has become a widely discussed concept in the context of metabolic health, especially when excess weight intersects with cardiovascular conditions. In recent years, the relationship between body weight and heart health has gained deeper attention, not only from medical communities but also from patients seeking to understand how these two areas influence one another. Rather than being viewed as separate concerns, obesity and heart disease are increasingly understood as interconnected elements within a complex physiological system.
At its core, Bariatric Surgery refers to surgical approaches aimed at altering the digestive system to support significant weight reduction. While traditionally associated with weight management, the conversation has expanded to include how these procedures interact with cardiovascular function. For individuals living with heart disease, this overlap raises important questions about safety, impact, and long term outcomes, making the topic both relevant and nuanced.
What makes this discussion particularly compelling is that heart disease itself is not a single condition. It includes a broad spectrum of issues such as coronary artery disease, hypertension, and structural heart changes. When combined with obesity, these conditions often amplify one another. As a result, Bariatric Surgery is no longer discussed only in terms of appearance or weight metrics, but as part of a broader metabolic and cardiovascular narrative.
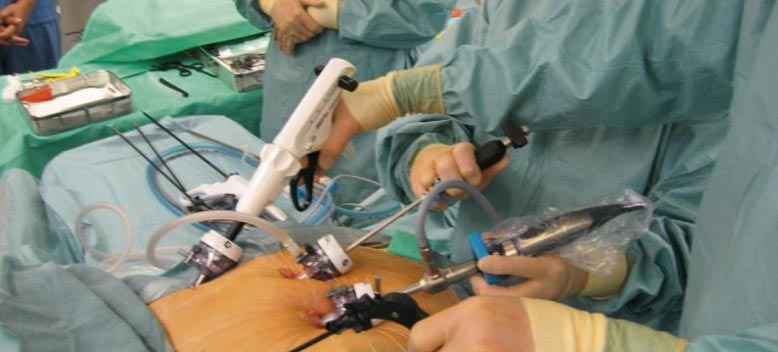
Bariatric Surgery and the Obesity Heart Connection
The link between excess body weight and heart disease is well established in scientific literature, yet it continues to evolve in interpretation. Obesity places additional strain on the cardiovascular system by increasing blood volume, altering lipid profiles, and influencing inflammatory pathways. Over time, these factors can contribute to the development or progression of heart related conditions.
Within this context, Bariatric Surgery enters the conversation as a potential turning point. Rather than addressing symptoms in isolation, it is often discussed as a systemic intervention that may influence multiple biological processes at once. Weight reduction following surgical intervention is frequently associated with changes in blood pressure regulation, glucose metabolism, and lipid balance, all of which are closely tied to heart health.
However, it is important to recognize that these associations are not uniform for everyone. Heart disease manifests differently across individuals, and so does the body’s response to weight loss. This variability is why discussions around Bariatric Surgery and heart disease often emphasize individualized evaluation rather than generalized conclusions.
How Bariatric Surgery Is Viewed in Cardiovascular Risk Discussions
In cardiovascular risk frameworks, body weight is often considered a modifiable factor. Unlike genetics or age, weight exists within a category that can change over time. Bariatric Surgery is frequently referenced in this space because it represents a structured and measurable approach to weight reduction, especially in cases where other strategies have not led to sustained results.
From a conceptual standpoint, the interest in Bariatric Surgery stems from its potential to alter risk trajectories rather than simply manage existing conditions. Research discussions often explore whether significant weight loss can shift long term cardiovascular outlooks. This includes examining patterns related to reduced strain on the heart muscle and improved vascular function.
At the same time, the presence of heart disease introduces additional layers of complexity. Surgical stress, anesthesia considerations, and recovery dynamics all become part of the equation. This is why Bariatric Surgery for patients with heart disease is usually framed as a multidisciplinary topic rather than a purely surgical one.
Bariatric Surgery Types and Their Broader Implications
Although the term Bariatric Surgery is often used as a single category, it actually includes several different procedural approaches. Each method interacts with the body in a distinct way, influencing digestion, absorption, and hormonal signaling. These differences matter when considering heart related conditions.
Some procedures focus primarily on restricting stomach capacity, while others combine restriction with changes in nutrient absorption. These variations can lead to different metabolic responses, which may indirectly affect cardiovascular markers. For example, shifts in insulin sensitivity or cholesterol metabolism are often discussed in relation to specific surgical techniques.
Rather than ranking these procedures, discussions around Bariatric Surgery and heart disease tend to explore how each option fits into a broader health profile. The goal is not to define a universal best choice, but to understand how different approaches align with individual cardiovascular contexts.
Psychological and Emotional Dimensions of Bariatric Surgery
Beyond physiology, Bariatric Surgery also carries psychological significance, particularly for individuals managing chronic heart conditions. Living with heart disease often involves ongoing monitoring, lifestyle adjustments, and emotional stress. The prospect of surgical weight loss can evoke a mix of hope, uncertainty, and caution.
Many patients view Bariatric Surgery as a symbolic reset, not just physically but mentally. It can represent a shift toward reclaiming agency over one’s health narrative. At the same time, heart disease can heighten concerns around risk and recovery, shaping how individuals emotionally approach the decision.
This emotional layer is increasingly recognized in modern health discussions. Rather than separating mental and physical health, Bariatric Surgery is often discussed as part of an integrated experience that includes motivation, perception, and long term self relationship.
Bariatric Surgery in a Changing Medical Landscape
Medical perspectives on Bariatric Surgery have evolved significantly over the past decades. What was once considered a last resort is now examined through a more nuanced lens, particularly in relation to chronic conditions like heart disease. Advances in surgical techniques, anesthesia, and perioperative care have all contributed to this shift.
At the same time, heart disease management has also progressed, with improved diagnostic tools and treatment strategies. The intersection of these advancements creates a dynamic space where Bariatric Surgery is evaluated not in isolation, but alongside broader cardiovascular care pathways.
This evolving landscape encourages ongoing research and discussion rather than fixed conclusions. For patients with heart disease, the relevance of Bariatric Surgery lies in how it fits into a larger, continuously adapting understanding of metabolic and cardiovascular health.
Bariatric Surgery and Observed Cardiovascular Trends
Bariatric Surgery is frequently discussed in academic and clinical settings through the lens of observed trends rather than absolute outcomes. Many observational studies explore how significant weight reduction coincides with changes in cardiovascular markers over time. These discussions often focus on patterns such as shifts in blood pressure ranges, lipid profiles, and inflammatory indicators that are commonly associated with heart disease.
What makes these observations compelling is their consistency across different populations. While individual responses vary, large scale analyses often highlight parallel trends between reduced body mass and altered cardiovascular stress factors. In this context, Bariatric Surgery is viewed less as a direct treatment for heart disease and more as a potential influence on the broader metabolic environment in which heart conditions exist.
It is also important to note that these trends are typically discussed with caution. Researchers emphasize correlation rather than causation, acknowledging that multiple variables evolve simultaneously after surgical weight loss. This balanced framing helps maintain scientific integrity while still recognizing why Bariatric Surgery remains central in cardiovascular conversations.
Bariatric Surgery and Metabolic Interactions
The metabolic dimension of Bariatric Surgery plays a key role in why it is often mentioned alongside heart disease. Metabolism influences how the body processes glucose, fats, and hormones, all of which have downstream effects on cardiovascular function. Weight reduction achieved through surgical means is frequently associated with changes in these metabolic pathways.
Insulin sensitivity, for example, is a recurring theme in discussions about Bariatric Surgery. Altered glucose regulation is closely linked to cardiovascular risk, and shifts in this balance are often examined after surgery. These metabolic interactions help explain why the topic extends beyond weight alone and enters the realm of systemic health.
Rather than presenting these changes as guaranteed outcomes, scientific discussions frame them as tendencies observed across cohorts. This approach reinforces the idea that Bariatric Surgery interacts with complex biological systems, making it a subject of ongoing analysis rather than definitive claims.
Bariatric Surgery in Multidisciplinary Evaluation Models
Patients with heart disease are rarely evaluated through a single lens. Instead, multidisciplinary models are often emphasized, bringing together perspectives from cardiology, metabolic science, and behavioral health. Within these frameworks, Bariatric Surgery is considered one component among many rather than a standalone solution.
These models highlight how surgical weight loss intersects with medication use, lifestyle patterns, and long term monitoring. For individuals with cardiovascular conditions, this integrated perspective helps contextualize Bariatric Surgery within a broader health narrative. It becomes part of a coordinated approach rather than an isolated intervention.
This multidisciplinary emphasis also shapes how risks and benefits are discussed. Rather than focusing on extremes, conversations around Bariatric Surgery often center on balance, timing, and individual context. This reflects a shift toward more nuanced decision making in modern healthcare.
Bariatric Surgery and Risk Perception
Risk perception plays a significant role in how Bariatric Surgery is understood by patients with heart disease. Surgical procedures naturally carry a sense of seriousness, and existing cardiovascular conditions can heighten awareness of potential complications. As a result, discussions often focus on how risk is assessed and interpreted rather than simply quantified.
From a psychological standpoint, Bariatric Surgery can be seen as both an opportunity and a source of concern. Some individuals associate it with proactive health management, while others focus on surgical stress and recovery challenges. This dual perception underscores why transparent, balanced information is central to the topic.
Importantly, modern discussions emphasize that risk is not static. Advances in surgical methods and perioperative care have reshaped how Bariatric Surgery is evaluated over time. This evolving perspective contributes to more informed and less polarized conversations.
Bariatric Surgery and Quality of Life Narratives
Beyond clinical markers, quality of life narratives are increasingly present in discussions about Bariatric Surgery. For patients with heart disease, daily experiences such as mobility, energy levels, and social participation often shape how health decisions are perceived. Weight related limitations can intersect with cardiovascular symptoms, creating layered challenges.
In this context, Bariatric Surgery is sometimes discussed in relation to lifestyle adaptation rather than purely medical outcomes. Observational reports often describe changes in daily routines and self perception following weight reduction. These narratives do not replace clinical data, but they add depth to the overall understanding.
Quality of life discussions also highlight subjectivity. What feels meaningful to one person may differ for another. This reinforces why Bariatric Surgery is rarely framed as a universal answer, but rather as an option whose value depends on individual priorities and experiences.
Bariatric Surgery and Long Term Observation
Long term observation is a critical element in how Bariatric Surgery is evaluated, especially for individuals with chronic conditions like heart disease. Short term changes may capture attention, but sustained patterns over years provide more meaningful insights. Researchers often focus on how weight stability, metabolic markers, and cardiovascular indicators evolve together.
These long term perspectives emphasize continuity rather than immediate transformation. Bariatric Surgery is discussed as part of an ongoing health journey rather than a single event. This framing aligns with how heart disease itself is managed, often requiring continuous adjustment rather than definitive resolution.
By viewing Bariatric Surgery through a long term lens, discussions remain grounded and realistic. The emphasis shifts from quick outcomes to sustained balance, reinforcing why the topic continues to hold relevance in cardiovascular health discourse.
Bariatric Surgery Advantages for Patients With Heart Disease
Bariatric Surgery is often discussed in relation to heart disease because of the broader advantages associated with substantial weight reduction. Rather than focusing on a single outcome, conversations usually highlight a cluster of potential benefits that emerge over time. These advantages are frequently framed as supportive factors that may influence overall cardiovascular burden.
One commonly mentioned advantage of Bariatric Surgery is how it can alter the physical demands placed on the heart. Reduced body mass may change how the cardiovascular system responds to daily activity, movement, and rest. This shift is not described as a cure, but rather as a change in context that may ease certain physiological pressures.
Another perceived advantage lies in systemic balance. Weight loss achieved through Bariatric Surgery is often associated with changes in inflammation markers and metabolic regulation. These systemic shifts help explain why the topic remains relevant in heart disease discussions without positioning surgery as a direct cardiac intervention.
Bariatric Surgery Limitations and Ongoing Debates
Despite its potential advantages, Bariatric Surgery is equally defined by its limitations. Scientific and public discussions frequently stress that outcomes vary widely between individuals. Factors such as age, existing heart conditions, lifestyle patterns, and long term adherence all shape how results unfold.
Durability is a recurring topic in debates around Bariatric Surgery. While initial weight reduction can be significant, maintaining long term balance often requires continuous adaptation. This reality keeps conversations grounded and avoids overly optimistic narratives.
There is also ongoing discussion about suitability. Bariatric Surgery is not framed as universally appropriate, particularly for individuals with complex cardiovascular profiles. These limitations reinforce why careful evaluation and realistic framing are central to responsible discourse.
Bariatric Surgery and Ethical Considerations
Ethical perspectives add another layer to how Bariatric Surgery is discussed for patients with heart disease. At the core of these conversations is the balance between potential benefit and individual autonomy. People are encouraged to consider not only physical factors but also personal values and long term expectations.
From an ethical standpoint, Bariatric Surgery raises questions about timing and intention. Is the goal weight reduction, improved quality of life, or broader metabolic change. These questions do not have universal answers, which is why ethical discussions remain open ended.
Transparency also plays a key role. Ethical frameworks emphasize clear communication about uncertainty, variability, and long term commitment. This approach ensures that Bariatric Surgery is discussed as a choice rather than an obligation.
Bariatric Surgery in Modern Health Narratives
In modern health narratives, Bariatric Surgery is increasingly positioned as part of a spectrum rather than a standalone milestone. Media, academic writing, and patient stories often frame it as one chapter within a longer health story.
This narrative shift reflects broader cultural changes. Health is no longer viewed purely through outcomes, but through experience, sustainability, and alignment with personal goals. Within this context, Bariatric Surgery becomes a tool that may support change rather than define it.
The language used around Bariatric Surgery has also evolved. Instead of dramatic transformation, discussions now emphasize adaptation, continuity, and balance. This framing resonates strongly with individuals managing chronic conditions such as heart disease.
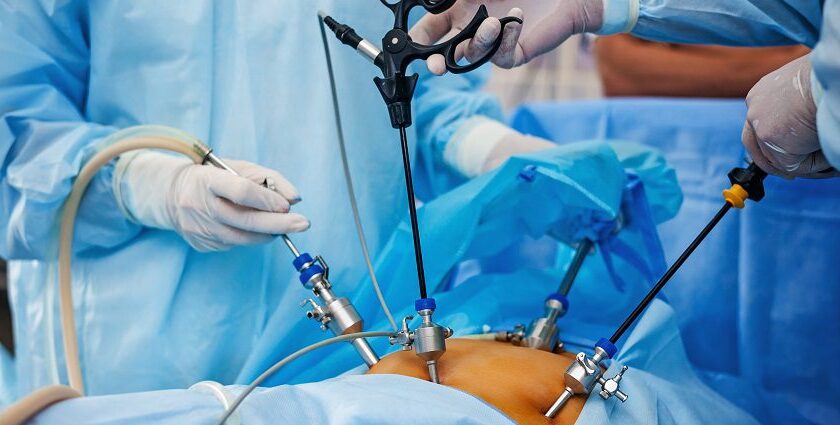
Bariatric Surgery and Decision Making Frameworks
Decision making frameworks surrounding Bariatric Surgery often highlight process over outcome. Rather than focusing solely on what may happen after surgery, attention is placed on how decisions are formed and evaluated.
These frameworks typically involve weighing physical, emotional, and social factors together. For patients with heart disease, this integrated approach helps situate Bariatric Surgery within real life complexity rather than abstract theory.
Importantly, modern frameworks avoid binary thinking. Bariatric Surgery is not positioned as right or wrong, but as context dependent. This nuanced perspective supports more informed and less pressured choices.
Bariatric Surgery as Part of a Long Term Perspective
Viewed over time, Bariatric Surgery is often described as a long term consideration rather than a single turning point. Its relevance lies in how it interacts with evolving health needs, personal priorities, and lifestyle patterns.
For individuals with heart disease, this long term view feels especially important. Chronic conditions rarely follow linear paths, and health decisions must adapt accordingly. Bariatric Surgery fits into this reality as an option that may influence trajectory rather than determine destiny.
Ultimately, the enduring discussion around Bariatric Surgery reflects its complexity. It sits at the intersection of science, psychology, ethics, and lived experience. This multifaceted role ensures that it remains a meaningful topic in conversations about heart disease, weight, and modern health decision making.