When it comes to bariatric surgery, Duodenal Switch vs Gastric Sleeve is a debate that frequently arises among patients and surgeons alike. Both procedures aim to reduce weight and improve metabolic health, yet they achieve these goals in different ways. Understanding their mechanisms, benefits, and long-term effects can help anyone curious about which surgery might provide more effective weight loss.

Understanding Duodenal Switch vs Gastric Sleeve Procedures
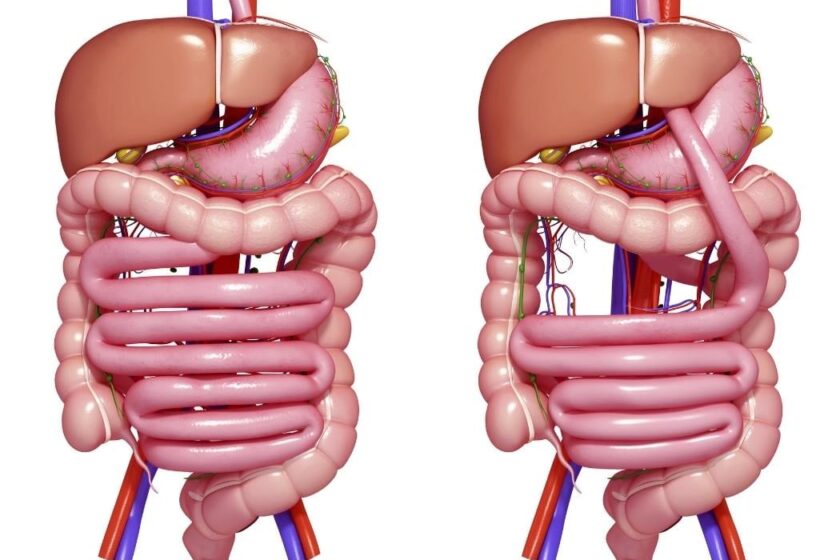
The first step in this comparison is understanding what each procedure entails. Duodenal Switch is a combination of restrictive and malabsorptive techniques. It reduces stomach size like a sleeve and reroutes a large portion of the small intestine, which limits calorie absorption. On the other hand, the Gastric Sleeve primarily focuses on restriction by removing a large portion of the stomach, leaving a narrow “sleeve” that reduces food intake and hunger hormones like ghrelin.
While both surgeries reduce weight, Duodenal Switch vs Gastric Sleeve differ fundamentally in their approach. The Duodenal Switch emphasizes nutrient malabsorption, which can lead to more rapid weight loss but requires stricter long-term dietary management. The Gastric Sleeve is less complex and carries fewer nutrient deficiencies, but its weight loss is generally slower.
Weight Loss Outcomes: Duodenal Switch vs Gastric Sleeve
Studies consistently show that Duodenal Switch vs Gastric Sleeve has distinct differences in long-term weight loss results. Research published in the Obesity Surgery Journal indicates that patients undergoing Duodenal Switch can lose 70-80% of their excess body weight within two years. In contrast, Gastric Sleeve patients often see a reduction of 50-60% in the same period.
| Procedure | Average Excess Weight Loss | Timeframe | Risk of Nutrient Deficiency |
| Duodenal Switch | 70-80% | 24 months | High |
| Gastric Sleeve | 50-60% | 24 months | Moderate |
The table highlights that while the Duodenal Switch tends to achieve more dramatic results, it also requires careful monitoring of vitamins, minerals, and protein intake. This factor is crucial when evaluating Duodenal Switch vs Gastric Sleeve effectiveness beyond mere weight numbers.
Metabolic and Health Benefits
When discussing Duodenal Switch vs Gastric Sleeve, it is important to consider their impact on metabolic health. The Duodenal Switch is known for its profound effects on type 2 diabetes remission and cholesterol management. By bypassing a significant portion of the small intestine, insulin sensitivity improves markedly.
The Gastric Sleeve also contributes to better metabolic profiles but mainly through weight reduction and hormonal changes. For patients with severe diabetes or metabolic syndrome, the Duodenal Switch may offer superior benefits, which further emphasizes the functional differences in Duodenal Switch vs Gastric Sleeve outcomes.
Surgical Complexity and Recovery
Surgical complexity is another critical factor in the Duodenal Switch vs Gastric Sleeve comparison. Duodenal Switch is technically more demanding and has a longer operative time. Recovery may involve a hospital stay of 3-5 days, with careful dietary progression.
The Gastric Sleeve is simpler, often performed laparoscopically, and patients usually go home within 1-2 days. This difference in recovery timelines affects not only patient preference but also overall procedure risk assessment. Understanding the balance between effectiveness and complexity is key to evaluating Duodenal Switch vs Gastric Sleeve for individual cases.
Nutritional Considerations and Lifestyle Changes
One cannot ignore the nutritional consequences when comparing Duodenal Switch vs Gastric Sleeve. Because the Duodenal Switch involves significant malabsorption, patients must commit to lifelong supplementation of vitamins A, D, E, K, calcium, and iron. Protein intake must also be monitored to prevent muscle loss.
Gastric Sleeve patients also require vitamin supplementation, but deficiencies are less severe. These factors highlight that weight loss surgery is not only a physical intervention but a lifestyle commitment, which is central to any discussion on Duodenal Switch vs Gastric Sleeve.
Long-Term Sustainability and Risks
Long-term success is another crucial aspect. Evidence suggests that Duodenal Switch vs Gastric Sleeve differs in sustainability. While Duodenal Switch patients maintain higher weight loss over 10-15 years, they are more prone to nutritional deficiencies, dumping syndrome, and gastrointestinal complications.
Gastric Sleeve patients experience slower weight regain but face fewer severe complications. For those evaluating surgery, understanding long-term risk vs reward is essential when comparing Duodenal Switch vs Gastric Sleeve.
Who Should Consider Each Procedure?
Patient selection is critical in the Duodenal Switch vs Gastric Sleeve debate. Duodenal Switch is generally recommended for patients with a BMI over 50 or those with severe metabolic diseases who can adhere to strict post-operative guidelines. The Gastric Sleeve is suitable for patients with a BMI of 35-50, moderate metabolic issues, or those seeking less invasive procedures.
Choosing the right surgery requires a careful evaluation of medical history, lifestyle, and weight loss goals, making the decision highly individualized within the context of Duodenal Switch vs Gastric Sleeve.
In the ultimate analysis of Duodenal Switch vs Gastric Sleeve, the choice depends on a combination of weight loss goals, metabolic health, surgical risk tolerance, and commitment to post-operative lifestyle changes. The Duodenal Switch provides more rapid and dramatic weight loss, with stronger metabolic benefits but higher risks and nutritional demands. The Gastric Sleeve offers a less complex surgery with moderate weight loss and fewer nutritional concerns.
Patients considering these surgeries must weigh the long-term implications, not just the immediate results, to make an informed decision. Understanding the nuanced differences in Duodenal Switch vs Gastric Sleeve ensures that expectations align with reality, optimizing outcomes and patient satisfaction.