The journey of Mini Gastric Bypass often begins with curiosity about how the body will respond after surgery. Many individuals search for reliable information about weight reduction patterns, recovery stages, and metabolic changes associated with this procedure. At its core, Mini Gastric Bypass represents a modern metabolic and bariatric intervention designed to help patients achieve substantial weight loss while maintaining relatively simplified surgical anatomy compared to traditional bypass techniques. At the clinic of Dr. Caynak, treatment planning focuses on long-term metabolic balance rather than only rapid scale changes.
The popularity of Mini Gastric Bypass has increased because it offers a combination of restriction and mild malabsorption mechanisms. Patients are often interested in understanding whether the results will feel natural and sustainable. Clinical observations suggest that weight reduction follows a gradual curve rather than an abrupt drop, allowing the body to adapt metabolically and hormonally. This balanced transformation is frequently considered one of the advantages of the technique.

Mini Gastric Bypass and Early Weight Loss Phase
After undergoing Mini Gastric Bypass, the early phase of weight reduction typically begins within the first few weeks. During this period, fluid balance changes, caloric intake decreases, and the stomach’s reduced capacity naturally limits portion size. Many patients notice visible changes around the abdomen and face as swelling subsides and fat metabolism shifts.
Scientific discussions around Mini Gastric Bypass suggest that initial weight loss may be faster than lifestyle-based dieting methods. However, early success should not be misinterpreted as the final outcome. The body undergoes complex hormonal adaptation following the surgery. Appetite-regulating signals such as ghrelin fluctuation and insulin sensitivity adjustment contribute to the evolving metabolic environment.
During the first three months after Mini Gastric Bypass, patients may lose a significant portion of their excess body weight. Exact numbers vary depending on preoperative body mass index, adherence to nutritional guidelines, and individual metabolic speed. Observational data from metabolic surgery centers show that many individuals achieve noticeable physical transformation during this stage.
Hydration management and protein intake are often emphasized in recovery programs. Although the surgical alteration helps restrict excessive calorie consumption, nutritional quality continues to influence the trajectory of weight reduction. Patients who maintain structured eating habits tend to observe more stable outcomes.
Mini Gastric Bypass Weight Loss Timeline: First Six Months
The six-month milestone is widely considered a critical checkpoint for Mini Gastric Bypass effectiveness. During this period, most patients experience the fastest proportional body mass reduction. Research trends in metabolic surgery suggest that nearly half to two-thirds of excess weight may be lost within the first half year for many candidates.
Metabolic recalibration plays a major role in this timeline. After Mini Gastric Bypass, insulin resistance may gradually improve, which can indirectly support fat utilization efficiency. Individuals with obesity-related metabolic disturbances sometimes report improvements in energy perception as the body shifts from glucose-dominant metabolism to more balanced energy sourcing.
Exercise integration during this period can amplify the outcome of Mini Gastric Bypass. Gentle cardiovascular movement supports muscle preservation while encouraging fat oxidation. Muscle mass maintenance is particularly important because rapid weight loss can occasionally lead to lean tissue reduction if protein consumption is inadequate.
Psychological adaptation is another subtle but important component of the process. Eating behavior changes after Mini Gastric Bypass may require conscious adjustment. Patients often learn to distinguish between physical hunger and habitual eating impulses, which contributes to long-term weight stability.
Long-Term Body Transformation After Mini Gastric Bypass
The long-term success of Mini Gastric Bypass is typically evaluated between 12 and 24 months after surgery. Weight loss tends to slow down as the body approaches a new equilibrium state. At this stage, metabolic efficiency improves and the risk of rapid rebound weight gain decreases when lifestyle consistency is maintained.
Hormonal balance alterations following Mini Gastric Bypass can also influence fat storage patterns. Some clinical observations indicate improvements in satiety signaling pathways. Patients frequently report feeling satisfied with smaller meals compared to their preoperative experience.
Another interesting aspect of Mini Gastric Bypass is its potential impact on obesity-related comorbidities. Blood sugar regulation, cardiovascular stress markers, and inflammatory indicators may show positive trends in many individuals. However, these biological responses vary according to genetic predisposition, age, and postoperative lifestyle management.
The durability of weight loss results depends largely on behavioral adaptation. The surgical modification provides a powerful biological tool, yet it does not replace conscious nutritional planning. Patients who integrate balanced macronutrient intake and moderate physical activity tend to preserve results more effectively.
Expected Weight Loss Numbers After Mini Gastric Bypass
Understanding expected numerical outcomes helps set realistic psychological expectations for Mini Gastric Bypass. On average, many clinical follow-ups report excess weight loss ratios between 60% and 85% within two years, although individual performance may vary.
The distribution of weight loss is not uniform across body regions. Visceral fat around abdominal organs often responds faster than subcutaneous fat layers. This phenomenon may explain why internal metabolic improvements sometimes appear before dramatic external appearance changes during the early months of Mini Gastric Bypass.
Body composition monitoring is more informative than scale measurement alone. Muscle-to-fat ratio changes can provide deeper insight into the true physiological impact of Mini Gastric Bypass. Some patients may experience slower scale reduction but still achieve healthy metabolic restructuring.
Age, baseline metabolic syndrome severity, and postoperative adherence all interact to influence outcome curves. Therefore, predicting exact kilogram loss after surgery is scientifically difficult. Instead, clinicians usually focus on percentage-based excess weight reduction when evaluating success.
Recovery Experience and Lifestyle Adaptation After Mini Gastric Bypass
The recovery journey following Mini Gastric Bypass is often described as a progressive lifestyle redesign rather than a short medical episode. The stomach’s reduced volume encourages mindful eating patterns. Many patients naturally transition toward slower chewing and smaller portion consumption.
Nutritional supplementation may become a long-term consideration after Mini Gastric Bypass because altered digestive pathways can affect micronutrient absorption. Iron, vitamin B12, and certain fat-soluble vitamins are frequently monitored during follow-up appointments.
Emotional and social adaptation also plays a subtle role. Eating is not only a biological activity but also a cultural and psychological experience. Individuals undergoing Mini Gastric Bypass sometimes discover new dietary preferences and develop different social dining habits.
Physical activity is generally introduced gradually. Walking is often the first recommended movement because it supports circulation without imposing excessive mechanical stress on the body. Over time, exercise intensity may be adjusted according to endurance improvement.
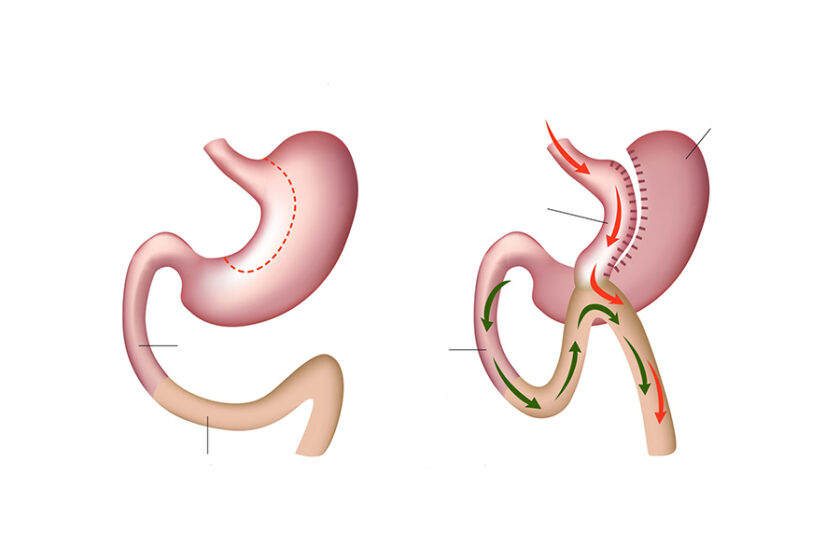
Who Is the Ideal Candidate for Mini Gastric Bypass?
Candidate selection is a fundamental factor influencing success rates of Mini Gastric Bypass. Individuals with severe obesity who have not achieved long-term results through conventional weight management approaches may benefit from the procedure.
Metabolic conditions such as type 2 diabetes sometimes motivate consideration of Mini Gastric Bypass. The procedure may assist in improving glycemic control by modifying gastrointestinal hormone signaling. However, surgical intervention is usually evaluated after comprehensive medical assessment.
Age is not an absolute barrier, but physiological resilience matters. Patients should be able to tolerate anesthesia and postoperative recovery processes. Nutritional awareness and willingness to follow long-term dietary guidance are also essential behavioral requirements.
At the practice of Dr. Caynak, evaluation includes metabolic history analysis, psychological readiness assessment, and anatomical suitability examination before recommending Mini Gastric Bypass.
Realistic Expectations from Mini Gastric Bypass
Mini Gastric Bypass offers a structured path toward meaningful body weight transformation, but the journey unfolds gradually rather than dramatically overnight. Early weight loss generally appears within the first months, followed by a more stabilized metabolic adjustment phase. Long-term results depend on how well surgical benefits are supported by lifestyle consistency.
The procedure stands out as a balanced metabolic surgery option for individuals seeking sustainable obesity management. Scientific observations suggest that when postoperative guidance is respected, Mini Gastric Bypass may help patients move toward healthier body composition and improved quality of life.
Weight reduction is only one dimension of the outcome. Energy perception, metabolic markers, and psychological comfort also contribute to overall satisfaction. For this reason, treatment planning and follow-up care remain essential components of the process.