Duodenal Switch surgery is widely recognized as one of the most effective procedures for significant weight loss and metabolic improvement. However, like any major surgical intervention, it carries a set of risks and potential complications that patients must carefully consider. Understanding these factors not only empowers patients to make informed decisions but also prepares them for the lifestyle adjustments required post-surgery.
Understanding the Basics of Duodenal Switch
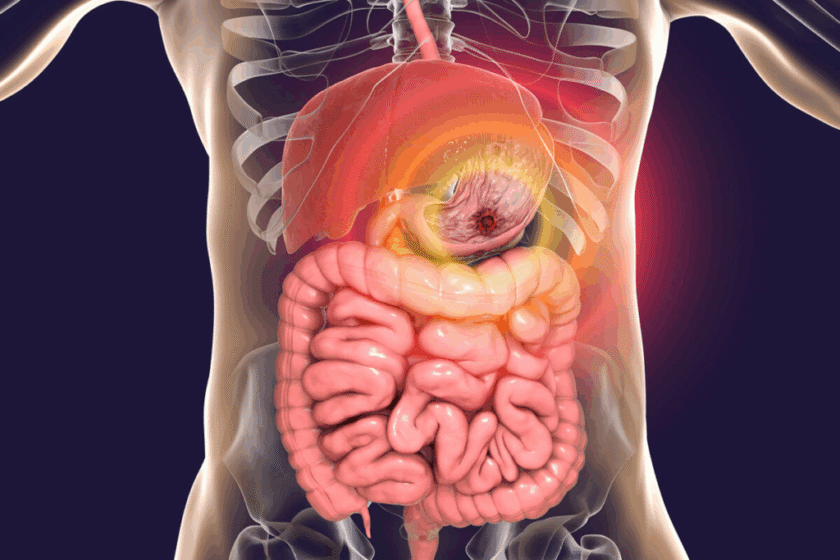
The Duodenal Switch procedure is a combination of restrictive and malabsorptive techniques. It involves reducing the stomach size and rerouting a significant portion of the small intestine. This dual approach helps patients achieve substantial weight loss, particularly in cases of severe obesity. Unlike simpler bariatric surgeries, the Duodenal Switch affects nutrient absorption, which is why the risk profile is more complex.
Patients often ask why this surgery is considered both effective and high-risk. The answer lies in its intricate nature: by reducing the stomach and bypassing much of the intestine, the body experiences profound metabolic changes. This can be highly beneficial for managing conditions such as type 2 diabetes, but it also introduces challenges in nutrient balance and digestive stability.
Short-Term Risks of Duodenal Switch
Short-term risks refer to complications that may occur during or shortly after surgery. The most common issues include:
- Infections – Surgical site infections or intra-abdominal infections can occur despite sterile techniques.
- Bleeding – Internal bleeding is a risk inherent to any major surgery.
- Leaks – Connections between the stomach and intestine (anastomoses) may leak, causing serious complications.
- Blood Clots – Postoperative immobility can increase the risk of deep vein thrombosis or pulmonary embolism.
While these risks sound alarming, careful preoperative assessment, experienced surgical teams, and modern perioperative care reduce their occurrence significantly. According to studies published in bariatric surgery journals, short-term complications occur in approximately 5–10% of patients, often manageable with timely intervention.
Long-Term Nutritional Complications
A critical aspect of Duodenal Switch surgery is its impact on nutrient absorption. The malabsorptive component, while contributing to effective weight loss, can lead to deficiencies:
- Fat-soluble vitamins (A, D, E, K) often require lifelong supplementation.
- Protein malnutrition may develop if dietary intake is insufficient.
- Mineral deficiencies, including calcium and iron, are common.
Patients must adopt a strict supplementation regimen and regular follow-ups with nutritionists. Research shows that adherence to supplementation protocols dramatically reduces the incidence of severe deficiencies and associated complications.
Digestive and Gastrointestinal Challenges
Digestive issues are frequently reported after Duodenal Switch surgery. These include:
- Diarrhea or fatty stools due to reduced fat absorption.
- Gastroesophageal reflux or bloating, particularly if dietary habits are not adjusted.
- Risk of small bowel obstruction, although relatively rare, can require surgical correction.
Interestingly, studies indicate that gradual adaptation of dietary patterns significantly mitigates these symptoms. High-protein, low-simple carbohydrate diets and small frequent meals help maintain digestive comfort.
Surgical and Mechanical Complications
Beyond physiological changes, mechanical complications can occur:
- Stricture formation at the surgical sites may cause narrowing of the digestive tract.
- Hernias at incision sites or internal herniation of intestines may arise.
- Anastomotic ulcers, though less common, require prompt treatment to prevent severe consequences.
Early detection is key, which is why routine follow-ups and awareness of unusual symptoms are essential. Prompt imaging and interventions can prevent minor issues from escalating.
Metabolic and Hormonal Implications
The Duodenal Switch procedure significantly alters hormonal signaling in the gut, affecting appetite regulation and glucose metabolism. While these changes often improve conditions like type 2 diabetes, they may also create challenges:
- Hypoglycemia can occur due to rapid nutrient absorption and insulin response.
- Changes in bile acid flow may affect cholesterol metabolism and liver function.
- Rapid weight loss can sometimes lead to gallstone formation.
Understanding these metabolic implications is vital for both patients and healthcare providers. Studies highlight the importance of monitoring blood glucose levels and liver function tests post-surgery.
Psychological and Lifestyle Considerations
Finally, the success and safety of Duodenal Switch surgery extend beyond medical procedures. Psychological readiness and lifestyle adjustments are crucial:
- Adapting to new eating patterns requires commitment and consistent follow-up.
- Emotional challenges, including body image adjustment and coping with rapid weight loss, are common.
- Long-term adherence to supplementation and monitoring prevents complications from escalating.
Clinicians emphasize a multidisciplinary approach, including counseling, nutrition guidance, and support groups, to optimize outcomes.
While Duodenal Switch surgery offers unparalleled benefits for severe obesity and metabolic disorders, it is not without risks. Short-term surgical risks, long-term nutritional challenges, digestive adjustments, mechanical complications, and metabolic changes all require careful consideration. Patients must engage with experienced bariatric teams, adhere to rigorous follow-up schedules, and embrace lifestyle changes to minimize complications.
Ultimately, informed decision-making, proactive management, and continuous monitoring transform potential risks into manageable challenges, ensuring the Duodenal Switch journey leads to sustained health benefits and improved quality of life.